CHRONIC KIDNEY DISEASE (CKD) IS A CONDITION CHARACTERIZED BY A GRADUAL LOSS OF KIDNEY FUNCTION OVER TIME.
What is chronic kidney disease (CKD)?
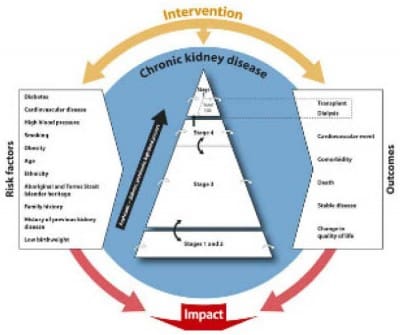
Chronic kidney disease occurs when a person suffers from permanent loss of kidney function. This happens gradually, usually from months to years.
Chronic kidney disease is divided into five stages of increasing severity (see below). The term “renal” refers to the kidney, so another name for kidney failure is “renal failure.” Mild kidney disease is often called renal insufficiency.
If kidney disease gets worse, high levels of waste can build up in your blood and make you feel sick. You may develop complications like high blood pressure, anemia (low blood count), weak bones, poor nutritional health and nerve damage. Also, kidney disease increases your risk of having heart and blood vessel disease.
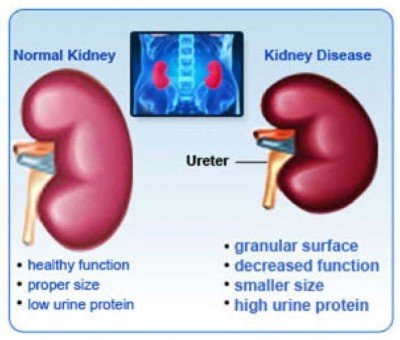
These problems may happen slowly over a long period of time. Chronic kidney disease may be caused by diabetes, high blood pressure and other disorders. Early detection and treatment can often keep chronic kidney disease from getting worse. When the disease progresses, it may eventually lead to kidney failure, which requires dialysis or a kidney transplant to maintain life.
The Facts about Chronic Kidney Disease (CKD)
- 26 million American adults have CKD and millions of others are at increased risk.
- Early detection can help prevent kidney disease from progressing to kidney failure.
- Heart disease is the major cause of death for all people with CKD.
- Glomerular filtration rate (GFR) is the best estimate of kidney function.
- Hypertension causes CKD and CKD causes hypertension.
- Persistent proteinuria (protein in the urine) means CKD is present.
- High risk groups include those with diabetes, hypertension and a family history of kidney disease.
- African-Americans, Hispanics, Pacific Islanders, Native Americans and seniors are at increased risk.
- Three simple tests can detect CKD: blood pressure, urine albumin and serum creatinine.
How common is Chronic Kidney Disease?
Chronic kidney disease is a growing health problem in the United States. A report by the Centers for Disease Control (CDC) determined that 16.8 percent of all adults over the age of 20 have chronic kidney disease. Thus, one in six individuals has kidney disease.
Anyone can get chronic kidney disease at any age. However, some people are more likely than others to develop it. If you have any of the following conditions, you are at a higher-than-normal risk of developing CKD and your kidney functions may need to be monitored regularly:

- Diabetes mellitus type 1 or 2
- High blood pressure
- Heart disease
- Liver disease
- Amyloidosis
- Sickle cell disease
- Systemic Lupus erythematous
- Vascular diseases such as arteritis, vasculitis, or fibromuscular dysplasia
- Vesicoureteral reflux (a urinary tract problem in which urine travels the wrong way back toward the kidney)
- Require regular use of anti-inflammatory medications
- A family history of kidney disease
- Patients with kidney transplant
- Have a family history of chronic kidney disease
- Are more than 65 years old
- Belong to a population group that has a high rate of diabetes or high blood pressure, such as African-Americans, Hispanic Americans, Asian, Pacific Islanders, and American Indians
What causes CKD?
Although chronic kidney disease sometimes results from primary diseases of the kidneys themselves, the major causes are diabetes and high blood pressure.
- Type 1 and Type 2 diabetes mellitus cause a condition called diabetic nephropathy, which is the leading cause of kidney disease in the United States.
- High blood pressure (hypertension), if not controlled, can damage the kidneys over time.
- Glomerulonephritis is the inflammation and damage of the filtration system of the kidneys, which can cause kidney failure. Postinfectious conditions and lupus are among the many causes of glomerulonephritis.
- Polycystic kidney disease is an example of a hereditary cause of chronic kidney disease wherein both kidneys have multiple cysts.
- Use of pain relievers, such as acetaminophen (Tylenol) and ibuprofen (Motrin, Advil, Aleve, Naproxen, etc.) regularly over long durations of time can cause analgesic nephropathy, another cause of kidney disease. Certain other medications can also damage the kidneys.
- Clogging and hardening of the arteries (atherosclerosis) leading to the kidneys causes a condition called ischemic nephropathy, which is another cause of progressive kidney damage.
- Obstruction of the flow of urine by stones, an enlarged prostate, strictures (narrowing), or cancers may also cause kidney disease.
- Other causes include HIV infection, sickle-cell disease, heroin abuse, amyloidosis, kidney stones, chronic kidney infections, and certain cancers.
- Malformations that occur as a baby develops in its mother’s womb. For example, a narrowing may prevent normal urination and cause urine to flow back up to the kidney. This causes infections and may damage the kidneys.
- Repeated urinary infections
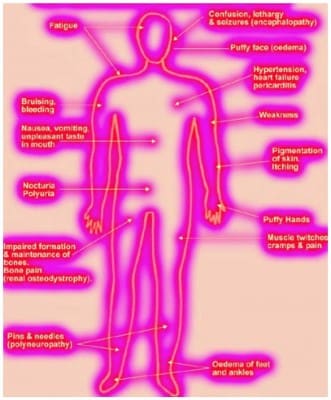
What are the symptoms of CKD?
The kidneys are remarkable in their ability to compensate for problems in their function. That is why chronic kidney disease may progress without symptoms for a long time until only very minimal kidney function is left.
Because the kidneys perform so many functions for the body, kidney disease can affect the body in a large number of ways. Symptoms vary greatly. Several different body systems may be affected. Notably, most patients have no decrease in urine output even with very advanced chronic kidney disease. However, you may notice that you:
- Feel more tired and have less energy.
- Have trouble concentrating.
- Have a poor appetite.
- Have trouble sleeping.
- Have muscle cramping at night.
- Have swollen feet and ankles.
- Have puffiness around your eyes, especially in the morning.
- Need to urinate more often, especially at night.
- Have decreased urinary production.
- Need to urinate frequently, especially at night (nocturia).
- Have swelling of the legs and puffiness around the eyes (fluid retention).
- Have high blood pressure.
- Have fatigue and weakness (from anemia or accumulation of waste products in the body).
- Have a loss of appetite, nausea, and vomiting.
- Have excessive itching, easy bruising, and pale skin (from anemia).
- Experience shortness of breath from fluid accumulation in the lungs.
- Have headaches, numbness in the feet or hands (peripheral neuropathy), disturbed sleep, altered mental status (encephalopathy from the accumulation of waste products or uremic poisons), and restless legs syndrome.
- Have chest pain due to pericarditis (inflammation around the heart).
- Bleed easily (due to poor blood clotting).
- Experience bone pain and fractures.
- Have decreased sexual interest and erectile dysfunction.
How Chronic Kidney Disease (CKD) Can Be Graded
GFR—glomerular filtration rate is the best test to measure your level of kidney function and determine your stage of chronic kidney disease as specified below. Your doctor can calculate it from the results of your blood creatinine test, your age, race, gender and other factors.

The earlier kidney disease is detected, the better the chance of slowing or stopping its progression.
Chronic Kidney Disease Diagnosis
Chronic kidney disease usually causes no symptoms in its early stages. Only lab tests can detect any developing problems. Anyone at increased risk for chronic kidney disease should be routinely tested for development of this disease.
- Urine, blood, and imaging tests (ultrasounds or CT scans) are used to detect kidney disease, as well as to follow its progress.
- All of these tests have limitations. They are often used together to develop a picture of the nature and extent of the kidney disease.
- In general, this testing can be performed on an outpatient basis.
Urine Tests
Urinalysis: A lot can be learned by analyzing the urine. The first step in urinalysis is doing a dipstick test. The dipstick has reagents that check the urine for the presence of various normal and abnormal constituents including protein. Then, the urine is examined under a microscope to look for red and white blood cells and the presence of casts and crystals (solids).
Only minimal quantities of albumin (protein) are present in urine normally. Therefore, a positive result on a dipstick test is abnormal. A more sensitive test is a laboratory estimation of the urine albumin (protein) and creatinine in the urine. The ratio of albumin and creatinine in the urine provides a good estimate of daily (protein) excretion.
24-Hour urine tests:
This test requires you to collect all of your urine for 24 consecutive hours. The urine may be analyzed for protein and waste products (urea nitrogen and creatinine). The presence of protein in the urine indicates kidney damage. The amount of creatinine and urea excreted in the urine can be used to calculate the level of kidney function and the glomerular filtration rate (GFR).
Glomerular filtration rate (GFR):
The GFR is a standard means of expressing overall kidney function. As kidney disease progresses, GFR falls. The normal GFR is about 100-140 mL/min in men and 85-115 mL/min in women. It decreases in most people with age. The GFR may be calculated from the amount of waste products in the 24-hour urine test or by using special markers administered intravenously. An estimation of the GFR (eGFR) can be calculated from the patient’s routine blood tests. Patients are divided into five stages of chronic kidney disease based on their GFR.
BLOOD TESTS
Creatinine and Urea (BUN) in the blood:
Blood urea nitrogen and serum creatinine are the most commonly used blood tests to screen for and monitor renal disease. Creatinine is a product of normal muscle breakdown. Urea is the waste product of breakdown of protein. The level of these substances rises in the blood as kidney function worsens.
Estimated GFR (eGFR):
The laboratory or your physician may calculate an estimated GFR using the information from your blood work. It is important to be aware of your estimated GFR and stage of chronic kidney disease. Your physician uses this information to recommend additional testing and suggestions for management.
Electrolyte levels and acid-base balance:
Kidney dysfunction causes imbalances in electrolytes, especially potassium, phosphorus, and calcium. High potassium (hyperkalemia) is a particular concern. The acid-base balance of the blood is usually disrupted as well.
Decreased production of the active form of vitamin D can cause low levels of calcium in the blood. The inability to excrete phosphorus due to failing kidneys causes its levels in the blood to rise. Testicular or ovarian hormone levels may also be abnormal.
Blood cell counts:
Because kidney disease disrupts blood cell production and shortens the survival of red cells, the red blood cell count and hemoglobin may be low (anemia). Some patients may also have iron deficiency due to blood loss in their gastrointestinal system. Other nutritional deficiencies may also impair the production of red cells.
OTHER TESTS
Ultrasound:
Ultrasound is often used in the diagnosis of kidney disease. An ultrasound is a noninvasive type of imaging test. In general, kidneys are shrunken in size in chronic kidney disease, although they may be normal or even large in size in cases caused by adult polycystic kidney disease, diabetic nephropathy, and amyloidosis. Ultrasound may also be used to diagnose the presence of urinary obstruction or kidney stones and also to assess the blood flow into the kidneys.
Biopsy

A sample of the kidney tissue (biopsy) is sometimes required in cases in which the cause of the kidney disease is unclear. Usually, a biopsy can be collected using local anesthesia by introducing a needle through the skin into the kidney. This is usually done as an outpatient procedure, though some institutions may require an overnight hospital stay.